Complementary and Alternative Therapies for Breast Cancer Worldwide
Affiliation
Department of Biomedical Sciences, International College of Business and Technology (ICBT), No 36, De Krester Place, Colombo- 04, Sri Lanka
Corresponding Author
Ms. Luxmiga Tharmarajah, Lecturer, Department of Biomedical Sciences, International College of Business and Technology (ICBT), No 36, De Krester Place, Colombo- 04, 00400, Sri Lanka, Tel: +94 773405413; Fax : +94 114 203 170; E-mail: luxmigat@gmail.com
Citation
Thamarajah L. Complementary and Alternative Therapies for Breast Cancer Worldwide. (2018) Lett Health Biol Sci 4(1): 27- 32.
Copy rights
© 2018 Thamarajah L. This is an Open access article distributed under the terms of Creative Commons Attribution 4.0 International License.
Keywords
Complementary and alternative medicine; Effectiveness, Quality; Regulation; Retrospective or cross-sectional studies; Safety; Traditional medicine
Abstract
Breast cancer is the second most common disease diagnosed and second leading cause of cancer death among women worldwide. Due to the failure of conventional healthcare, patients’ prefer for “holistic” or “natural” remedy which plays an active role in their treatment supporting of the body’s own healing powers and the desire for a non-toxic, gentle treatment. World health organization (WHO) evaluates one-third of the world’s population like Africa, Asia and Latin America as no regular access to modern medicines, but rich resources of traditional remedies are available and accessible. However, a considerable number of breast cancer patients, even those who live in North America and Western Europe also have searched for other options and, reported to use various types of Complementary and Alternative Medicine (CAM). CAM is a group of various medical and health care systems practices, their origins come from outside of mainstream medicine. CAM has begun to find a place in cancer treatment and helps the patients to cope with disease symptoms and side effects of treatment to improve their quality of life. According to survivor CAM use is common among worldwide breast cancer patients. CAM therapies are necessary for physicians and other healthcare practitioners to help patients make better and easy choices. Many of the patients are discussing CAM therapy options with their physicians. However, a subgroup of patients using many alternative therapies seems to have great adjustment problems. Immediate research is needed to systematically estimate the efficiency and safety of CAM use, mainly for the use of herbal medicines.
Introduction
Cancer is fast in replacing heart disease as it is the number one cause of death in adults worldwide[1]. Breast cancer is the second most common disease diagnosed and second top form of cancer death among women. Breast cancers develop either in the breast tissue made up of glands for milk or in the lobes. Breast cancer is seen either during a screening checkup, before symptoms have developed, or after a woman discovered a lump[2]. In most countries, including China, United States, India, Sri Lanka, America, Germany standard treatment choices for breast cancer include surgical methods, chemotherapy, radiotherapy, and endocrine therapy. For a century, cancer experts have been continuing on the same route of treatment for a majority of cancer cases which are unlikely to make many positive results in the lives of their patients, therefore patients all over the world are in search of better choices[1]. Due to the failure of conventional healthcare, patients’ prefer for “holistic” or “natural” remedy which plays an active role in their treatment supporting of the body’s own healing powers and the desire for a non-toxic, gentle treatment[3]. Holistic medicine means they seek to restore health and balance to the “whole person” not just the body they focus on your mind, emotions, and spirit, too. Complementary and Alternative Medicine (CAM) is a form of holistic remedy[4].
The meaning of complementary and alternative medicine within the past 20 years has revived to include a range of behavioral methods (e.g., spiritual techniques and relaxation methods) and clinical methods (such as massage, herbal remedies, and chiropractic) which were previously not been considered as the components of alternative medicine. Now surveys have found that 30 to 40 percent of the U.S. public uses alternative medicine. A study using the National Health Interview Survey (NHIS) documented that spiritual therapy yoga, chiropractic, and osteopathic manipulation are the most common CAM remedies used by breast cancer patients[5]. Retrospective or cross-sectional studies have studied that the use of alternative medicine among the cancer patients population are large. Mutually, these studies have proven that level of income, amount of education, and age are all strongly predictive of the level of use of alternative medicine, which includes mind therapies such as hypnosis, mental imagery, and relaxation and body therapies such as acupuncture, herbal treatments and chiropractic[6].
For thousands of years, Traditional medicines play a primary role in people’s health. 42% of the population in the USA, 48% in Australia, 70% in Canada and 77% in Germany uses CAM. Therapies and practices vary from country to country and from region to region, the most familiar are Ayurveda the traditional Indian medicine (TIM) and Traditional Chinese Medicine (TCM). These systems of treatments now have spread to other countries. Some countries such as: In the United States, interest in alternative therapies is growing steadily such treatments are, metabolic therapy, diets, mega-vitamins, mental imagery for anti-tumor effects, spiritual or faith healing and immune therapy are most commonly used. In a united states Survey of 2,055 adults showed that 42% of the defendants to use CAM are more women than men and in 15 million adults, or 18.4% of all prescription drug users, combined complementary prescription drugs with herbal remedies and/or high-dose vitamins[7]. In Germany and Switzerland, mistletoe preparations (Viscum album) a semi-parasitic plant that is used to cure cancer are most repeatedly applied. Nutrition-related measures, such as special drinks, teas or diets, and vitamin preparations, are used often. In many cases, combinations of two or more preparations are used simultaneously[3]. In China breast cancer patients are believed to be using Traditional Chinese Medicine (TCM) and/or other CAM therapies, TCM usually consisting of herbal medicine and acupuncture. Ayurveda medicine, unani and homeopathy is widely practiced in Sri Lanka and India[8]. In Saudi Arabia, a cross-sectional study among 518 participants, 35.7% used Hijama (wet cupping) and 22% used massage therapy[5].
Development of Complementary and Alternative Medicine (CAM)
World health organization (WHO) evaluates one-third of the world’s population like Africa, Asia and Latin America as no regular access to modern medicines, however rich resources of traditional remedies are available and accessible[4]. Even breast cancer patients those who live in North America and Western Europe also have searched for other options and, reported to use various types of Complementary and Alternative Medicine (CAM)[8]. In Ayurveda, the most ancient living traditions are TIM and TCM remain.Globally the interest in traditional medicine has increased. Interest of Public to CAM is high due to increased side effects in conventional treatment, lack of curative therapies for several chronic diseases and high cost of new drugs and microbial resistance. Pharmaceutical companies have improved their approaches in favor of natural drug product improvement and discovery. For example, in Europe, based on natural product chemistry AnalytiCon Discovery has stressed on drug discovery. In the Asia-Pacific region, MerLion Pharmaceuticals in Singapore has inclusive structures and skills necessary to produce natural product-based drug discovery[9].
China over the world has grandly supported its own remedies with a science-based method, while Ayurveda still needs more widespread scientific research and science-based evidence. The Pharmaceutical Research and Development Committee report of Ministry of Chemicals, Government of India also highlights the reputation of traditional information[9].
Types of complementary and alternative medicine therapies
Herbal Therapies: Herbal and botanical treatments, many of this has been used by some cultures for hundreds of years, and today 25% of the source are used by the Western pharmaceutical drugs. In Chinese medicine, for example, individual or mixtures of plants and herbs are generally arranged to restore balance and increase or decrease energy. Common herbs and botanical treatments used in the United States include garlic oil for the treatment of mild hypertension, Echinacea for improving the immune system, and herbs for controlling symptoms related to menopause and pregnancy[10].
Homeopathy was founded in the late 1800s by a German physician, Samuel Hahnemann, found that “a substance that produces a certain set of symptoms in a healthy person has the influence to cure a sick person revealing those same symptoms”. Homeopathic drugs are very watery doses of plant, animal, or mineral substances that seek to cure signs of health problems by encouraging the body’s immune system to fight the illness[10]. Homeopathic remedies are accessible over the counter without prescriptions. If a statement were to state that a homeopathic therapy could treat a serious disease, such as cancer, by U.S. law, it could be traded by prescription only. Systematic reviews and meta-analyses of homeopathy clinical trials show no final proof that homeopathic remedies are in effect for any medical condition[11].
Mental therapies: Meditation and relaxation techniques are psychologic techniques that are used to calm the body and mind by aiming attention on different objects, a repeated word or mantra, an image, or by body and breathing workouts. These techniques shows a distinct biochemical changes in the body, including the lowering of blood pressure, pulse rates, and levels of stress hormones in the blood[12].
Guided imagery and visualization are psychologic techniques that involve generating a mental image or method to represent bodily jobs to give individuals a sense of control over their illness. Chronic diseases are treated including cancer. Spiegel found that patients with breast cancer who used guided imagery and other counseling methods had a survival time that was twice that of control subjects who did not take any such remedies[10].
Hypnosis is a psychologic method that involves the generation of a positive mental state of healing and the use of therapeutic idea. Sometimes patients are educated self-hypnosis to apply to themselves when the problem repeats[13].
Biofeedback is a psychologic method that uses a variety of monitoring machines that deliver feedback to the patient about how the body is responding to mental control. It has been used to treat conditions associated to stress and hypertension[12].
Spiritual healing is a method in which one directs entreaties to a Supreme Being, a Universal Power, or God. This practice involves a state of prayerfulness, a feeling of genuine caring, compassion, love, or empathy with the target system or a feeling that the individual is “one” with the Supreme Being[10].
Physical therapies: Acupuncture is a technique used in traditional Chinese medicine and is often used in combination with herbal treatments. Consist of insertion of tiny needles at certain points on the body highpoint to direct the flow of energy, or chi, to certain organs and try to restore health. Acupuncturists help patient’s stability the chi energy within and between the five major organ systems: the heart, lungs, liver, spleen, and kidneys[10]. Modern versions consist of electrical pulses (electro-acupuncture) or laser (laser acupuncture) to provide extra encouragement modern research advises that the effect of acupuncture may be mediated by the release of neurotransmitters[14].
Acupressure is a type of acupuncture that consist of applying pressure with the fingers and thumbs, rather than needles, to chi points on the surface of the body. This technique relieves muscular tension and enables oxygen and nutrients to be spread to tissues throughout the body. Alike, reflexology involves applying pressure to particular chi points on the bottom of the feet[15].
Massage therapy, in the West, involves applying pressure with the fingers and hands to various parts of the body to reduce stress and relax muscle tension. Though, in Chinese they use this therapy to treat chronic illness and it is more and more used for symptom relief in patients with cancer[16].
Yoga, in Sanskrit means “union,” originated in India and includes stretching, breathing, and physical exercise to help the flow of energy and to create healing processes inside the body[12].
Tai Chi and Chi Gong, also part of traditional Chinese medicine, involve similar components. Relies more on technique than on physical prowess, tai chi is a form of breathing exercises also serve a meditative function, so reducing stress[15].
Chiropractic is found in USA at the end of 19th century by Daniel David Palmer. Chiropractic is associated between spine and nervous system and on the self-healing properties of human body[4].
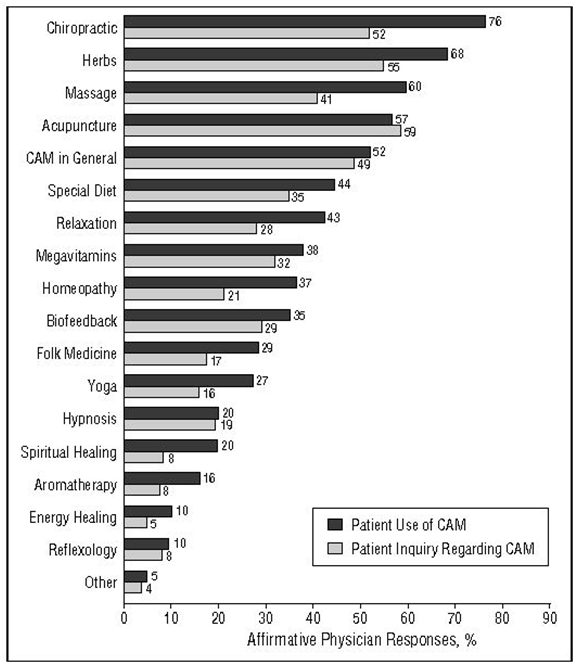
Osteopaths is treatment of manipulation and massage of skeleton and musculature. 15 Physicians report of patients using CAM and inquiry regarding CAM is shown in Figure 1.
Figure 1: Physician reports of patient use of and inquiries regarding complementary and alternative medicine (CAM). The top bar shows what percentage of physicians had at least 1 patient using that method, and the bottom bar shows the percentage of physicians who had been asked by patients about that method. All numbers indicate percentages of physicians[17].
Safety and Side Effects of CAM for Breast Cancer
Acupuncture helps to relieve hot flashes caused by some breast cancer treatments also includes less vomiting, pain, and fatigue but women with lymph nodes removed under one arm shouldn’t have acupuncture needles inserted into that arm if not a condition called lymphedema causes with risk of swelling and excess fluid[18]. Electro-acupuncture has advantage for chemotherapy-induced acute vomiting, but researches with national of the art antiemetic as well as research for refractory symptoms should decide clinical importance. Acupressure decrease chemotherapy-induced acute nausea severity, though researches did not involve a sample control[19].
In China, Chi gong is used as an addition to chemotherapy and radiation and as a primary treatment for patients with advance cancer. In Table 1 More detail about CAM that is safe to use during chemotherapy is included. U.S. hospitals are offering tai chi as a complement to regular care. This can increase in self-esteem, a sense of well-being and an improvement in quality of life, since tai chi and chi gong are gentle the carry few risks[18].
Yoga increases energy and quality of life with breast cancer patients especially after surgery but for some women depending on the treatment more athletic styles of yoga, such as power yoga, work the upper body may not be good. If a patient had lymph nodes removed under one arm, there is a risk of lymphedema[20].
Antioxidants found in herds prevent or treats cancer but higher dose of supplements can be a risk to the body. Many of these “natural” products such as dietary supplements, herbal supplements, and vitamins are considered to be safe because they are present in, or produced by, nature. However, that is not true in all cases some may affect how well other medicines work in your body[18].
Meditation, journaling, music or art therapy and guided imagery, helps the cancer patients to relax mentally, make patients feel less alone and help create a positive mental and physical state[18].
In herbal treatment Public tends not to be conscious that herbs are dilute natural drugs that contain scores of different chemicals, most of which have not been acknowledged and their effects are not always expectable. Patients undergoing active treatment should be told to stop using herbal remedies, because some herbs cause tricky interactions with chemotherapeutic agents, dangerous blood pressure changes, sensitization of the skin to radiation therapy, and other unwanted interactions with anesthetics during surgery. The risk of herb-drug medications appears to be greatest for patients with kidney or liver problems[21]. Overall and common side effects for herbal treatments can be transient side-effects and they were all associated to ingesting herbs or minerals. Other side effects includes stomach aches (by using thyme and nettle tea, one with vitamin C, and one with aloe); gastric upset and nausea from using nettle tea; headaches and migraine; diarrhea; itching [by using nettle leaves, one with selenium tablets and one with Iscador (mistletoe)]; and poor renal status/accumulation of body acid (by using vitamin C)[22].
Table 1: CAM that is safe to use during chemotherapy.
| Mind-body therapy CAM | Supportive care use |
|---|---|
| Acupuncture* | • decreases acute vomiting caused by chemotherapy |
| Hypnosis* | • decreases nausea and vomiting caused by chemotherapy. |
| Imagery and relaxation (body relaxation combined with visualization e.g: imagining warm sun melting away cancer cells) | • Boosts immune functioning during treatment. |
| Massage* | • Decreases nausea and vomiting caused by chemotherapy • reflexology (foot massage) decreases anxiety during treatment. |
| Meditation (combines relaxation with self awareness, which brings the person into the moment, free from anxiety concerning the past or future) | • Alters immune patterns by decreasing stress • Decreases anxiety and depression. |
| Music | •reduces anxiety. |
The Effectiveness of CAM in Breast cancer
Some CAM treatments have been evaluated and found to be safe and effective. However there are some CAM treatments which are found to be ineffective or possibly harmful. Less is known about many CAM therapies, and research has been slower for a number of reasons:
• Time and funding issues
• Problems finding institutions and cancer researchers to work with on the studies
• Regulatory issues
CAM treatments need to be assessed with the same long and careful research process used to calculate conventional medical treatments that includes clinical trials with large numbers of patients[24]. When a patient does not choose a proper CAM treatment there are possible chances for failure in the treatment, this includes when Some patients might use ineffective alternative therapies instead of effective cancer treatments this limits their life and reducing their quality of life. Other patients might hire alternative treatments which cause straight harm; for this, there are numerous options; for instance, if the patients take self-medication without proper doctor’s prescription they would decrease the effectiveness of many mainstream medications, as well as some cancer drugs[25].
CAM treatment depends on safety, efficacy and quality
There has been very less method for scientific research into Complementary and Alternative Medicine used by cancer patients in spite of the outward widespread use of CAM. Randomized control trials (RCT) have been used as the unique rule in evaluating the effectiveness of a medical intervention and reliable proof in the form of systematic reviews and meta-analyses on the topic of safety and efficacy[26].
American Society of Clinical Oncology has reported against CAM, for its insufficient evidence base for CAM therapies, products and lack of peer-reviewed scientifically conducted research[26].
Other faults are: lack of international and national standards for ensuring safety, efficacy, and quality control, lack of acceptable regulation of herbal medicines, lack of registration of CAM providers, insufficient support of research and lack of research method[4].
Regulation of Practice and Practitioner
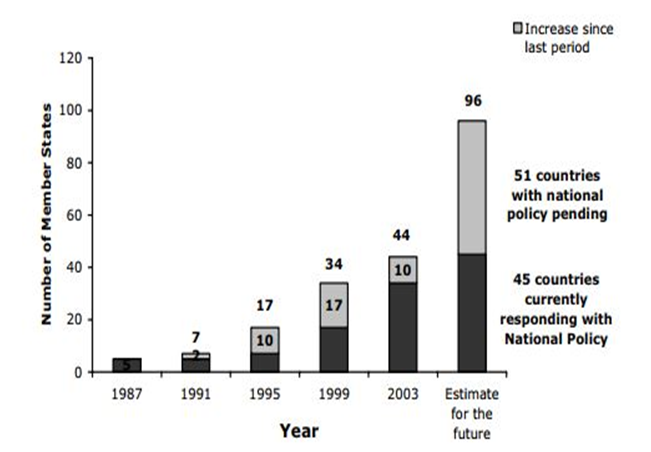
To reach combination of CAM into national health care programs and systems, one must decide qualified practitioners and practices. To accomplish this some counties has taken steps. Figure 2 represents the number of member states with national policies for CAM. In Great Britain the House of Lords Committee on Complementary Medicine suggested that self-regulation be a keystone for the validation of the complementary professions. In Great Britain, osteopaths (treatment of manipulation and massage of skeleton and musculature) and chiropractors (diagnosis and manipulative treatment of misalignments of the joints) have been registered as official health professionals through an action of Parliament, and the basis for maintenance of professional standards is self-regulation. For medical herbalists and acupuncturists similar principle is being applied, both of which are on path for registration in Great Britain. New Zealand has recorded more than 600 Maori traditional healers (they use herbal medicines and spiritual energy healings) who offer services within the wider health care system. Asia has appreciated the most progress in uniting traditional health systems into national health policy. In some Asian countries, such as China, has accomplished through national policy. In others (example, India and South Korea), alteration has come about as an outcome of politicization of the traditional medicine agenda. In the United States, acupuncturists are licensed in 41 states and chiropractors are licensed in all 50 states. The National Council for Authorization of Acupuncture and Oriental Medicine holds a national examination for traditional Chinese herbal medicine. The Botanical Medicine Academy and the American Herbalists Guild are rising a voluntary national exam for US practitioners of Western herbal medicine. The United States recently discussed greater national attention on the policy stadium with the launch in 2000 of the White House Commission on Complementary and Alternative Medicine Policy. The commission’s command was to provide “legislative and administrative recommendations for guaranteeing that public policy take full advantage of the benefits to Americans of Complementary and Alternative Medicine[4]. In Sri Lanka, 60% to 70% of the countryside population depends on traditional and natural remedy for their primary health care. In 1961 the Ayurveda Medical Council, include registration for Ayurveda practitioners, pharmacists, and nurses. In early 1980, the Ministry of Traditional Medicine was recognized as a separate department to be directed by a senior parliamentarian who is an Ayurveda consultant by profession. A central feature of the Ministry’s operation has been the establishment of traditional medical dispensaries and hospitals that provide medical care at no cost. The Cabinet Ministry for traditional Medicine was recognized in 1994, there was previously a State Minister for Traditional Medicine. Research and advance activities are undertaken on behalf of these governmental offices by the Department of Ayurveda and the Bandaranaike Memorial Ayurveda Research Institute[27].
Figure 2: Number of Member States with national policies on CAM. Member States with pending national policy on CAM are 51 countries which indicated that such policies are in the process of development. 45 countries currently responding with national policy. Countries with national policies, 44 provided the year in which the policy was issued. The number of Member States with national policies on CAM has increased significantly overall in the last decade. It is also obvious that a majority of Member States that responded (59%, 27 States) have issued such policies since 1996[4].
The Homeopathic Council is in charge for regulating and controlling the practice of homeopathic medicine and sustaining the Homeopathic Medical College. The Council is permitted to register and recognize homeopathic medical practitioners; recognize homeopathic teaching institutes, dispensaries, and hospitals; hold examinations and award degrees in homeopathic medicine and arrange for postgraduate study in homeopathy, only registered physicians may practice homeopathy for gain and use the title “Registered Homeopathic Practitioner” [27].
Role of oncologists when dealing with patients using CAM
Many cancer patients use complementary and alternative medicinal therapies; Patients appear increasingly enthusiastic to discuss the use of these medicines, especially when asked by their oncologists. In demand to encourage open communication of CAM use by their patients, oncologists should be educated about the most commonly used therapies, or at least be able to direct patients to trustworthy sources of data. Patients should be warned to avoid questionable alternative therapies in an accessible, evidence-based atmosphere. Many unproven alternatives are sponsored by a very appealing and convincing technique. Grooming the topic aside firmly without open discussion may not advise against patients’ use. On the other hand, complementary therapies that help manage pain, fatigue, nausea, anxiety, and other warning sign should be included into the patient’s overall care. In some cases, patients feel that problems they notice as important fail to obtain enough attention. Complementary therapies improve the physician-patient relationship patients’ qualities of life and patient satisfaction[11].
Breast cancer women use CAM to increase their immunity, prevent disease development, cure cancer or improve their quality of life. The Quality of Life may be termed as the sense of well-being involving social, mental, physical and spiritual characteristics of the person[5].
Conclusion
CAM is a developing field in health care and in mainly among breast cancer patients, Studies show the use of CAM during cancer is only a small number of patients completely take out from all conventional medicine, instead, most patients combine CAM with their biomedical routine. Cancer patients who are using or considering using CAM should talk with their doctor or nurse. Some therapies may mingle with conventional medical treatment or even be harmful. It is also a good idea to learn whether the therapy has been proven to cure cancer. Physicians particularly oncologists should have the knowledge of CAM. Oncologists should be willing to confer the role of CAM with their patients and cheer patients to participate in CAM. Since CAM is extensively used nowadays, the healthcare team may need to discuss the practice of CAM with breast cancer women and be up to date on the aids and hazard of CAM use through well-equipped training programs and workshops.
Many CAM treatments lack good scientific evidence of their safety and effectiveness. Studies are underway to determine the safety and efficacy of many CAM agents and practices for cancer patients. Due to The limitations of CAM studies, there are potential problems in interactions of conventional medicine and CAM and the lack of systematic evidence about how and when women with breast cancer choose to use CAM and to decide whether or not to include complementary therapy in their treatment. An area in which particular care is needed is on both medical staff and complementary counselors in the area of eatable medicines, such as herbal medicines and antioxidants. The growing use of traditional remedies demands more scientifically sound proof for the principles behind remedies and for the success of medicines.
Use of chemotherapy appears to be related with the relative frequency use of CAM therapies, which may point out that it was used during chemotherapy to release symptoms. Further analysis is needed to identify which CAM therapies are being used and under what conditions. Certification of the effectiveness of these treatments for various signs should become a high primacy.
Acknowledgement: The authors wish to thank the authorities of International College of Business and Technology (ICBT) campus for their support and encouragement to write this paper.
Competing Interests: The authors declare that they have no competing interests, financially or otherwise.
References
- 1. Michael, l. Beating cancer with natural medicine. (2003) Health and Fitnes 270.
Pubmed||Crossref||Others
- 2. Hider, P., Nicholas, B. The early detection and diagnosis of breast cancer : a literature review – a n update. (1999) NZHTA REPORT 2(2): 1-11.
Pubmed||Crossref||Others
- 3. Richter, R., Fleischhacker, W. W., Sperner-unterweger, B.‘Use of alternative / complementary therapy in breast cancer patients – a psychological perspective. (2001) Sup C cancer 9(4): 267-274.
- 4. Bodeker, G., Kronenberg, F. A public health agenda for traditional, complementary, and alternative medicine. (2002) Am J Public Health 92(10): 1582-1591.
- 5. Albabtain, H., Alwhaibi, M., Alburaikan, K., et al. Quality of life and complementary and alternative medicine use among women with breast cancer. (2018) Saudi Pharma J 26(3): 416-421.
Pubmed||Crossref ||Others
- 6. Burstein, H. J., Gelber, S., Guadagnoli, E., et al. Use of Alternative Medicine by Women with Early-Stage Breast Cancer. (1999) Nejm 340(22): 1733-1739.
- 7. Lambe, C. E. Complementary and Alternative Therapy Use During Treatment of Breast Cancer. (2006) sch of N 3-172.
Pubmed||Crossref||Others
- 8. Cui, Y., Shu, X.O., Gao, Y., et al. Use of complementary and alternative medicine by Chinese women with breast cancer. (2004) Breast Cancer Res Treat 85(3): 263-270.
- 9. Patwardhan, B., Warude, D., Bhatt, N., et al. Ayurveda and traditional Chinese medicine: A comparative overview(2005) Evid based Complementary Alternat Med 2(4) 465-473.
- 10. Lee, M.M., Linn, S.S., Alder, S.R., et al. Alternative Therapies Used by Women With Breast Cancer in Four Ethnic Populations. (2000) J Natl Cancer Inst 92(1): 42- 47.
- 11. Barrie, R. C., Gary, D., Complementary and Alternative Therapies for Cancer. (2003) The oncologist 9(1): 80-89.
- 12. Barnett, J. E., Shale, A. J. The integration of complementary and alternative medicine (CAM) into the practice of psychology: A vision for the future (2012) Professional Psychology 43(6): 576-585.
- 13. Montgomery, G. H. David, D., Weltz, C.R., et al. A randomized clinical trial of a brief hypnosis intervention to control side effects in breast surgery patients (2007) J Natl Cancer Inst 99(17): 1304-1312.
- 14. Cassileth, B.R., Deng, G. Complementary and Alternative Therapies for Cancer. (2004) Oncologist 9(1): 80-89.
- 15. Cassileth, B. R. The Complete Guide to Complementary Therapies in Cancer Care. (2011).
Pubmed||Crossref||Others
- 16. Cassileth, B. R. Vickers, A. J. Massage Therapy for Symptom Control : Outcome Study at a Major Cancer Center. (2004) j pain symman 28(3): 244-249.
- 17. Corbin Winslow, L., Shapiro, H. Physicians Want Education About Complementary and Alternative Medicine to Enhance Communication With Their Patients. (2002) Arch Intern Med 162(10): 1176-1181.
- 18. Melinda Ratini, D. Complementary Treatments for Breast Cancer. (2015) wedmb 3.
Pubmed||Crossref||Others
- 19. Ezzo, J. Allen, C., Zhang, G., et al. Acupuncture-point stimulation for chemotherapy-induced nausea and vomiting. (2005) J Clin Oncol 23(28): 7188-7198.
- 20. Jaqueline, L. The Gale Encyclopedia Of Alternative Medicine. (2005)
Pubmed||Crossref||Others
- 21. Adriane,F.B. Herb-drug interactions. (2000) the lancet 355 (9198): 134-138.
- 22. Molassiotis, A. Ozden, G.,Magri, M., et al. Use of complementary and alternative medicine in cancer patients: a European survey. (2005) Ann Oncol 16(4): 655-663.
- 23. Peter, J. S., Alexandra, C., Jeremy L., et al. What complementary and alternative medicine ( CAM ) can I safely use with chemotherapy ? (2016) Sunshine Coast Hospital and Health Service: 1-8.
Pubmed||Crossref||Others
- 24. Ferreira, L. M., Complementary and Alternative Medicine. (2015) prostate news today.
Pubmed||Crossref||Others
- 25. Edzard, E. Cancer patients who use alternative medicine die sooner. (2003) united states.
Pubmed||Crossref||Others
- 26. Mariama, A., Andrew, P. J. The use of complementary and alternative medicine by cancer patients. (2007) NCBI 10(4).
- 27. Legal Status of Traditional Medicine and Complementary / Alternative Medicine : A Worldwide Review. (2001) WHO 200.
Pubmed||Crossref||Others